- Have any questions?
- 085913 90567
- drgeorgechestdiseases@gmail.com
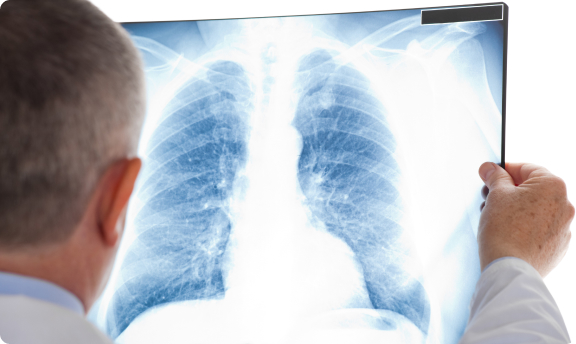
How Is Pleural Effusion Diagnosed and Treated ?

Esophageal Cancer Surgery Survival Rate?
May 12, 2026
What are Mediastinal Tumor Symptoms and is Surgery Needed?
May 14, 2026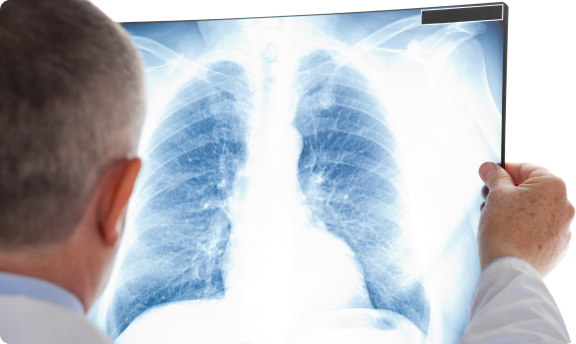
Pleural effusion is fluid accumulation in the pleural space between the lung and chest wall. Breathlessness is the most common symptom. Up to 25% of patients remain asymptomatic at diagnosis. Malignant pleural effusion carries a median survival of 3 to 12 months depending on the underlying cancer type.
According to Dr. George Karimundackal, one of the most experienced thoracic surgeons in Mumbai, pleural effusion is one of those conditions that patients and GPs both underestimate. By the time breathlessness is significant enough to prompt a referral, the effusion is often large enough that the lung has already started losing functional capacity.
What Are the Symptoms of Pleural Effusion?
Stage at Symptoms depend on how much fluid has accumulated and how quickly it developed. Small effusions are often completely silent. Larger ones produce a recognisable clinical picture that gets missed when the chest isn’t properly examined.
- Breathlessness is the most commonly reported symptom and the primary driver of referral. It worsens progressively as fluid accumulates and the lung loses functional capacity on the affected side.
- Chest pain or heaviness on the affected side, typically pleuritic in nature and worsening with deep inspiration or coughing. Often described as a dull pressure rather than the sharp pain patients expect.
Quarter of malignant pleural effusion patients have no symptoms at all when the diagnosis is made. The effusion shows up on a scan done for something completely unrelated. That’s actually more common than most people expect.
- Dry non-productive cough from fluid compressing the lower airways and triggering stretch receptors in the pleural lining. Distinct from the cough pattern seen in primary airway disease and easy to miss without imaging.
- Reduced activity levels, fatigue, and inability to lie flat. Orthopnoea from pleural effusion gets misattributed to cardiac failure regularly before the chest X-ray is done.
Read about chest wall surgery for conditions involving the pleural cavity and chest wall.
How Is Pleural Effusion Treated?
Treatment depends on the cause, effusion size, whether it is malignant, and how quickly fluid re-accumulates after initial drainage. Not every effusion needs intervention.
- Initial large-volume thoracocentesis aspirating 500 to 1,500 mL is the standard first intervention for symptomatic effusion. Around 25% of patients don’t improve symptomatically after drainage — those are the ones with non-expanding or trapped lung requiring a different pathway entirely.
Two definitive options after that. IPC or pleurodesis. Which one depends on whether the lung actually expands after the fluid comes out.
- Indwelling pleural catheter is a silicone tube inserted percutaneously with a one-way valve allowing intermittent home drainage. As effective as pleurodesis as first-line treatment for malignant effusion and the standard option for trapped lung where pleurodesis isn’t technically possible.
- Talc pleurodesis. Chemical fusion of the pleural surfaces to stop fluid coming back. Only works if the lung expands properly after drainage — which is why trapped lung rules it out entirely and IPC becomes the default instead.
- VATS decortication for complex loculated effusions and empyema where medical drainage has failed, and for non-expanding trapped lung where a thick fibrous peel is preventing re-expansion regardless of how much fluid is removed.
For further reading on pleural conditions and non-surgical treatment options read Empyema Treatment Without Surgery
Why Choose Dr. George Karimundackal for Pleural Effusion Treatment?
Before his current Director role at Nanavati Max Super Specialty Hospital, Dr. George Karimundackal was Professor of Thoracic Surgery at the Tata Memorial Hospital and manages the full spectrum of pleural disease including thoracocentesis, IPC insertion, VATS decortication, and talc pleurodesis.
Patients with pleural effusion ask similar questions at first consult. What the main symptom is breathlessness, which worsens as fluid increases and may not appear at all in small effusions. Whether it always needs draining no, asymptomatic effusions are often observed rather than immediately drained. How quickly it comes back depends entirely on the underlying cause because malignant effusions typically re-accumulate within weeks. And whether surgery is always needed not always, because IPC and pleurodesis manage most cases without open surgery.
FAQ
What are the main symptoms of pleural effusion?
Breathlessness. That’s the one that drives most referrals. Chest heaviness, dry cough, and fatigue are also common but often get attributed to other causes before imaging is done.
Does pleural effusion always need to be drained?
No. Up to 25% of malignant pleural effusion patients remain asymptomatic and are observed rather than drained.
What is the difference between IPC and pleurodesis for pleural effusion?
IPC allows home drainage via a permanent catheter. Pleurodesis fuses pleural surfaces to prevent fluid re-accumulation.
When does pleural effusion require surgery?
VATS decortication. When the effusion is loculated or the lung won’t expand after drainage because of a thick fibrous peel, medical management stops working and surgery is the only option left.
References
- NCBI PMC. Updates in Management of Malignant Pleural Effusion. https://pmc.ncbi.nlm.nih.gov/articles/PMC12433027/
- NCBI PMC. Malignant Pleural Effusion: Diagnosis and Treatment. https://pmc.ncbi.nlm.nih.gov/articles/PMC11593232/